-
 Specific Antimicrobial Activities Revealed by Comparative Evaluation of Selected Gemmotherapy Extracts
Specific Antimicrobial Activities Revealed by Comparative Evaluation of Selected Gemmotherapy Extracts -
 Comparison of Antibiotic Susceptibility Testing Results for Gram-Positive Mastitis Pathogens from Dairy Cows
Comparison of Antibiotic Susceptibility Testing Results for Gram-Positive Mastitis Pathogens from Dairy Cows -
 Jugiones A–D: Antibacterial Xanthone–Anthraquinone Heterodimers from Australian Soil-Derived Penicillium shearii CMB-STF067
Jugiones A–D: Antibacterial Xanthone–Anthraquinone Heterodimers from Australian Soil-Derived Penicillium shearii CMB-STF067
Journal Description
Antibiotics
Antibiotics
is an international, peer-reviewed, open access journal on all aspects of antibiotics, published monthly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, SCIE (Web of Science), PubMed, PMC, Embase, CAPlus / SciFinder, and other databases.
- Journal Rank: JCR - Q1 (Pharmacology & Pharmacy) / CiteScore - Q1 (General Pharmacology, Toxicology and Pharmaceutics)
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 13.7 days after submission; acceptance to publication is undertaken in 2.5 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
Impact Factor:
4.8 (2022);
5-Year Impact Factor:
4.9 (2022)
Latest Articles
Genetic Alternatives for Experimental Adaptation to Colistin in Three Pseudomonas aeruginosa Lineages
Antibiotics 2024, 13(5), 452; https://doi.org/10.3390/antibiotics13050452 - 15 May 2024
Abstract
Pseudomonas aeruginosa is characterized by a high adaptive potential, developing resistance in response to antimicrobial pressure. We employed a spatiotemporal evolution model to disclose the pathways of adaptation to colistin, a last-resort polymyxin antimicrobial, among three unrelated P. aeruginosa lineages. The P. aeruginosa
[...] Read more.
Pseudomonas aeruginosa is characterized by a high adaptive potential, developing resistance in response to antimicrobial pressure. We employed a spatiotemporal evolution model to disclose the pathways of adaptation to colistin, a last-resort polymyxin antimicrobial, among three unrelated P. aeruginosa lineages. The P. aeruginosa ATCC-27833 reference strain (Pa_ATCC), an environmental P. aeruginosa isolate (Pa_Environment), and a clinical isolate with multiple drug resistance (Pa_MDR) were grown over an increasing 5-step colistin concentration gradient from 0 to 400 mg/L. Pa_Environment demonstrated the highest growth pace, achieving the 400 mg/L band in 15 days, whereas it took 37 and 60 days for Pa_MDR and Pa_ATCC, respectively. To identify the genome changes that occurred during adaptation to colistin, the isolates selected during the growth of the bacteria (n = 185) were subjected to whole genome sequencing. In total, 17 mutation variants in eight lipopolysaccharide-synthesis-associated genes were detected. phoQ and lpxL/PA0011 were affected in all three lineages, whereas changes in pmrB were found in Pa_Environment and Pa_MDR but not in Pa_ATCC. In addition, mutations were detected in 34 general metabolism genes, and each lineage developed mutations in a unique set of such genes. Thus, the three examined distinct P. aeruginosa strains demonstrated different capabilities and genetic pathways of colistin adaptation.
Full article
Open AccessArticle
Eminent Antimicrobial Peptide Resistance in Zymomonas mobilis: A Novel Advantage of Intrinsically Uncoupled Energetics
by
Reinis Rutkis, Zane Lasa, Marta Rubina, Inese Strazdina and Uldis Kalnenieks
Antibiotics 2024, 13(5), 451; https://doi.org/10.3390/antibiotics13050451 - 15 May 2024
Abstract
Relative to several model bacteria, the ethanologenic bacterium Zymomonas mobilis is shown here to have elevated resistance to exogenous antimicrobial peptides (AMPs)—with regard to both peptide bulk concentration in the medium and the numbers of peptide molecules per cell. By monitoring the integration
[...] Read more.
Relative to several model bacteria, the ethanologenic bacterium Zymomonas mobilis is shown here to have elevated resistance to exogenous antimicrobial peptides (AMPs)—with regard to both peptide bulk concentration in the medium and the numbers of peptide molecules per cell. By monitoring the integration of AMPs in the bacterial cell membrane and observing the resulting effect on membrane energy coupling, it is concluded that the membranotropic effects of the tested AMPs in Z. mobilis and in Escherichia coli are comparable. The advantage of Z. mobilis over E. coli apparently results from its uncoupled mode of energy metabolism that, in contrast to E. coli, does not rely on oxidative phosphorylation, and hence, is less vulnerable to the disruption of its energy-coupling membrane by AMPs. It is concluded that the high resistance to antimicrobial peptides (AMPs) observed in Z. mobilis not only proves crucial for its survival in its natural environment but also offers a promising platform for AMP production and sheds light on potential strategies for novel resistance development in clinical settings.
Full article
(This article belongs to the Section Antimicrobial Peptides)
Open AccessArticle
Potential Surviving Effect of Cleome droserifolia Extract against Systemic Staphylococcus aureus Infection: Investigation of the Chemical Content of the Plant
by
Jawaher Alqahtani, Walaa A. Negm, Engy Elekhnawy, Ismail A. Hussein, Hassan Samy Hassan, Abdullah R. Alanzi, Ehssan Moglad, Rehab Ahmed, Sarah Ibrahim and Suzy A. El-Sherbeni
Antibiotics 2024, 13(5), 450; https://doi.org/10.3390/antibiotics13050450 - 15 May 2024
Abstract
The increasing rates of morbidity and mortality owing to bacterial infections, particularly Staphylococcus aureus have necessitated finding solutions to face this issue. Thus, we elucidated the phytochemical constituents and antibacterial potential of Cleome droserifolia extract (CDE). Using LC-ESI-MS/MS, the main phytoconstituents of CDE
[...] Read more.
The increasing rates of morbidity and mortality owing to bacterial infections, particularly Staphylococcus aureus have necessitated finding solutions to face this issue. Thus, we elucidated the phytochemical constituents and antibacterial potential of Cleome droserifolia extract (CDE). Using LC-ESI-MS/MS, the main phytoconstituents of CDE were explored, which were kaempferol-3,7-O-bis-alpha-L-rhamnoside, isorhamnetin, cyanidin-3-glucoside, kaempferide, kaempferol-3-O-alpha-L-rhamnoside, caffeic acid, isoquercitrin, quinic acid, isocitrate, mannitol, apigenin, acacetin, and naringenin. The CDE exerted an antibacterial action on S. aureus isolates with minimum inhibitory concentrations ranging from 128 to 512 µg/mL. Also, CDE exhibited antibiofilm action using a crystal violet assay. A scanning electron microscope was employed to illuminate the effect of CDE on biofilm formation, and it considerably diminished S. aureus cell number in the biofilm. Moreover, qRT-PCR was performed to study the effect of CDE on biofilm gene expression (cna, fnbA, and icaA). The CDE revealed a downregulating effect on the studied biofilm genes in 43.48% of S. aureus isolates. Regarding the in vivo model, CDE significantly decreased the S. aureus burden in the liver and spleen of CDE-treated mice. Also, it significantly improved the mice’s survival and substantially decreased the inflammatory markers (interleukin one beta and interleukin six) in the studied tissues. Furthermore, CDE has improved the histology and tumor necrosis factor alpha immunohistochemistry in the liver and spleen of the CDE-treated group. Thus, CDE could be considered a promising candidate for future antimicrobial drug discovery studies.
Full article
(This article belongs to the Special Issue Antibacterial, Antibiofilm and Anti-virulence Activity Research of Both Natural and Synthetic Products, 2nd Edition)
Open AccessArticle
The Tick Saliva Peptide HIDfsin2 TLR4-Dependently Inhibits the Tick-Borne Severe Fever with Thrombocytopenia Syndrome Virus in Mouse Macrophages
by
Luyao Wang, Yishuo Liu, Rui Pang, Yiyuan Guo, Yingying Ren, Yingliang Wu and Zhijian Cao
Antibiotics 2024, 13(5), 449; https://doi.org/10.3390/antibiotics13050449 - 15 May 2024
Abstract
Ticks transmit a variety of pathogens to their hosts by feeding on blood. The interactions and struggle between tick pathogens and hosts have evolved bilaterally. The components of tick saliva can directly or indirectly trigger host biological responses in a manner that promotes
[...] Read more.
Ticks transmit a variety of pathogens to their hosts by feeding on blood. The interactions and struggle between tick pathogens and hosts have evolved bilaterally. The components of tick saliva can directly or indirectly trigger host biological responses in a manner that promotes pathogen transmission; however, host cells continuously develop strategies to combat pathogen infection and transmission. Moreover, it is still unknown how host cells develop their defense strategies against tick-borne viruses during tick sucking. Here, we found that the tick saliva peptide HIDfsin2 enhanced the antiviral innate immunity of mouse macrophages by activating the Toll-like receptor 4 (TLR4) signaling pathway, thereby restricting tick-borne severe fever with thrombocytopenia syndrome virus (SFTSV) replication. HIDfsin2 was identified to interact with lipopolysaccharide (LPS), a ligand of TLR4, and then depolymerize LPS micelles into smaller particles, effectively enhancing the activation of the nuclear factor kappa-B (NF-κB) and type I interferon (IFN-I) signaling pathways, which are downstream of TLR4. Expectedly, TLR4 knockout completely eliminated the promotion effect of HIDfsin2 on NF-κB and type I interferon activation. Moreover, HIDfsin2 enhanced SFTSV replication in TLR4-knockout mouse macrophages, which is consistent with our recent report that HIDfsin2 hijacked p38 mitogen-activated protein kinase (MAPK) to promote the replication of tick-borne SFTSV in A549 and Huh7 cells (human cell lines) with low expression of TLR4. Together, these results provide new insights into the innate immune mechanism of host cells following tick bites. Our study also shows a rare molecular event relating to the mutual antagonism between tick-borne SFTSV and host cells mediated by the tick saliva peptide HIDfsin2 at the tick–host–virus interface.
Full article
(This article belongs to the Special Issue Peptide Antibiotics from Microbes and Venomous Animals, 2nd Edition)
►▼
Show Figures

Graphical abstract
Open AccessArticle
Colonization by Extended-Spectrum β-Lactamase-Producing Enterobacterales and Bacteremia in Hematopoietic Stem Cell Transplant Recipients
by
Luiza Arcas Gonçalves, Beatriz Barbosa Anjos, Bruno Melo Tavares, Ana Paula Marchi, Marina Farrel Côrtes, Hermes Ryoiti Higashino, Bruna del Guerra de Carvalho Moraes, José Victor Bortolotto Bampi, Liliane Dantas Pinheiro, Fernanda de Souza Spadao, Vanderson Rocha, Thais Guimarães and Silvia Figueiredo Costa
Antibiotics 2024, 13(5), 448; https://doi.org/10.3390/antibiotics13050448 - 15 May 2024
Abstract
Background: Assessing the risk of multidrug-resistant colonization and infections is pivotal for optimizing empirical therapy in hematopoietic stem cell transplants (HSCTs). Limited data exist on extended-spectrum β-lactamase-producing Enterobacterales (ESBL-E) colonization in this population. This study aimed to assess whether ESBL-E colonization constitutes a
[...] Read more.
Background: Assessing the risk of multidrug-resistant colonization and infections is pivotal for optimizing empirical therapy in hematopoietic stem cell transplants (HSCTs). Limited data exist on extended-spectrum β-lactamase-producing Enterobacterales (ESBL-E) colonization in this population. This study aimed to assess whether ESBL-E colonization constitutes a risk factor for ESBL-E bloodstream infection (BSI) and to evaluate ESBL-E colonization in HSCT recipients. Methods: A retrospective analysis of ESBL-E colonization and BSI in HSCT patients was conducted from August 2019 to June 2022. Weekly swabs were collected and cultured on chromogenic selective media, with PCR identifying the β-lactamase genes. Pulsed-field gel electrophoresis (PFGE) and whole-genome sequencing (WGS) assessed the colonizing strains’ similarities. Results: Of 222 evaluated HSCT patients, 59.45% were colonized by ESBL-E, with 48.4% at admission. The predominant β-lactamase genes were blaTEM (52%) and blaSHV (20%). PFGE analysis did not reveal predominant clusters in 26 E. coli and 15 K. pneumoniae strains. WGS identified ST16 and ST11 as the predominant sequence types among K. pneumoniae. Thirty-three patients developed thirty-five Enterobacterales-BSIs, with nine being third-generation cephalosporin-resistant. No association was found between ESBL-E colonization and ESBL-BSI (p = 0.087). Conclusions: Although the patients presented a high colonization rate of ESBL-E upon admission, no association between colonization and infection were found. Thus, it seems that ESBL screening is not a useful strategy to assess risk factors and guide therapy for ESBL-BSI in HSCT-patients.
Full article
(This article belongs to the Special Issue Colonization and Infection of Multi-Drug Resistant Organisms)
►▼
Show Figures

Figure 1
Open AccessArticle
Listeria monocytogenes from Food Products and Food Associated Environments: Antimicrobial Resistance, Genetic Clustering and Biofilm Insights
by
Adriana Silva, Vanessa Silva, João Paulo Gomes, Anabela Coelho, Rita Batista, Cristina Saraiva, Alexandra Esteves, Ângela Martins, Diogo Contente, Lara Diaz-Formoso, Luis M. Cintas, Gilberto Igrejas, Vítor Borges and Patrícia Poeta
Antibiotics 2024, 13(5), 447; https://doi.org/10.3390/antibiotics13050447 - 14 May 2024
Abstract
Listeria monocytogenes, a foodborne pathogen, exhibits high adaptability to adverse environmental conditions and is common in the food industry, especially in ready-to-eat foods. L. monocytogenes strains pose food safety challenges due to their ability to form biofilms, increased resistance to disinfectants, and
[...] Read more.
Listeria monocytogenes, a foodborne pathogen, exhibits high adaptability to adverse environmental conditions and is common in the food industry, especially in ready-to-eat foods. L. monocytogenes strains pose food safety challenges due to their ability to form biofilms, increased resistance to disinfectants, and long-term persistence in the environment. The aim of this study was to evaluate the presence and genetic diversity of L. monocytogenes in food and related environmental products collected from 2014 to 2022 and assess antibiotic susceptibility and biofilm formation abilities. L. monocytogenes was identified in 13 out of the 227 (6%) of samples, 7 from food products (meat preparation, cheeses, and raw milk) and 6 from food-processing environments (slaughterhouse-floor and catering establishments). All isolates exhibited high biofilm-forming capacity and antibiotic susceptibility testing showed resistance to several classes of antibiotics, especially trimethoprim-sulfamethoxazole and erythromycin. Genotyping and core-genome clustering identified eight sequence types and a cluster of three very closely related ST3 isolates (all from food), suggesting a common contamination source. Whole-genome sequencing (WGS) analysis revealed resistance genes conferring resistance to fosfomycin (fosX), lincosamides (lin), fluoroquinolones (norB), and tetracycline (tetM). In addition, the qacJ gene was also detected, conferring resistance to disinfecting agents and antiseptics. Virulence gene profiling revealed the presence of 92 associated genes associated with pathogenicity, adherence, and persistence. These findings underscore the presence of L. monocytogenes strains in food products and food-associated environments, demonstrating a high virulence of these strains associated with resistance genes to antibiotics, but also to disinfectants and antiseptics. Moreover, they emphasize the need for continuous surveillance, effective risk assessment, and rigorous control measures to minimize the public health risks associated to severe infections, particularly listeriosis outbreaks. A better understanding of the complex dynamics of pathogens in food products and their associated environments can help improve overall food safety and develop more effective strategies to prevent severe health consequences and economic losses.
Full article
(This article belongs to the Special Issue Rise of Antibiotic Resistance: Mechanisms Involved and Solutions to Tackle It)
►▼
Show Figures

Figure 1
Open AccessBrief Report
Characterization of Salmonella Phage P1-CTX and the Potential Mechanism Underlying the Acquisition of the blaCTX-M-27 Gene
by
Qiu-Yun Zhao, Run-Mao Cai, Ping Cai, Lin Zhang, Hong-Xia Jiang and Zhen-Ling Zeng
Antibiotics 2024, 13(5), 446; https://doi.org/10.3390/antibiotics13050446 - 14 May 2024
Abstract
The P1 phage has garnered attention as a carrier of antibiotic resistance genes (ARGs) in Enterobacteriaceae. However, the transferability of ARGs by P1-like phages carrying ARGs, in addition to the mechanism underlying ARG acquisition, remain largely unknown. In this study, we elucidated the
[...] Read more.
The P1 phage has garnered attention as a carrier of antibiotic resistance genes (ARGs) in Enterobacteriaceae. However, the transferability of ARGs by P1-like phages carrying ARGs, in addition to the mechanism underlying ARG acquisition, remain largely unknown. In this study, we elucidated the biological characteristics, the induction and transmission abilities, and the acquisition mechanism of the blaCTX-M-27 gene in the P1 phage. The P1-CTX phage exhibited distinct lytic plaques and possessed a complete head and tail structure. Additionally, the P1-CTX phage was induced successfully under various conditions, including UV exposure, heat treatment at 42 °C, and subinhibitory concentrations (sub-MICs) of antibiotics. Moreover, the P1-CTX phage could mobilize the blaCTX-M-27 gene into three strains of Escherichia coli (E. coli) and the following seven different serotypes of Salmonella: Rissen, Derby, Kentucky, Typhimurium, Cerro, Senftenberg, and Muenster. The mechanism underlying ARG acquisition by the P1-CTX phage involved Tn1721 transposition-mediated movement of blaCTX-M-27 into the ref and mat genes within its genome. To our knowledge, this is the first report documenting the dynamic processes of ARG acquisition by a phage. Furthermore, this study enriches the research on the mechanism underlying the phage acquisition of drug resistance genes and provides a basis for determining the risk of drug resistance during phage transmission.
Full article
(This article belongs to the Special Issue Antibiotic Residues, Antimicrobial Resistance and Intervention Strategies of Foodborne Pathogens, 2nd Edition)
►▼
Show Figures

Figure 1
Open AccessReview
Novel Siderophore Cephalosporin and Combinations of Cephalosporins with β-Lactamase Inhibitors as an Advancement in Treatment of Ventilator-Associated Pneumonia
by
Szymon Viscardi, Ewa Topola, Jakub Sobieraj and Anna Duda-Madej
Antibiotics 2024, 13(5), 445; https://doi.org/10.3390/antibiotics13050445 - 14 May 2024
Abstract
In an era of increasing antibiotic resistance among pathogens, the treatment options for infectious diseases are diminishing. One of the clinical groups especially vulnerable to this threat are patients who are hospitalized in intensive care units due to ventilator-associated pneumonia caused by multidrug-resistant/extensively
[...] Read more.
In an era of increasing antibiotic resistance among pathogens, the treatment options for infectious diseases are diminishing. One of the clinical groups especially vulnerable to this threat are patients who are hospitalized in intensive care units due to ventilator-associated pneumonia caused by multidrug-resistant/extensively drug-resistant Gram-negative bacteria. In order to prevent the exhaustion of therapeutic options for this life-threatening condition, there is an urgent need for new pharmaceuticals. Novel β-lactam antibiotics, including combinations of cephalosporins with β-lactamase inhibitors, are proposed as a solution to this escalating problem. The unique mechanism of action, distinctive to this new group of siderophore cephalosporins, can overcome multidrug resistance, which is raising high expectations. In this review, we present the summarized results of clinical trials, in vitro studies, and case studies on the therapeutic efficacy of cefoperazone-sulbactam, ceftolozane-tazobactam, ceftazidime-avibactam, and cefiderocol in the treatment of ventilator-associated pneumonia. We demonstrate that treatment strategies based on siderophore cephalosporins and combinations of β-lactams with β-lactamases inhibitors show comparable or higher clinical efficacy than those used with classic pharmaceuticals, like carbapenems, colistin, or tigecycline, and are often associated with a lower risk of adverse events.
Full article
(This article belongs to the Special Issue Antimicrobial Activity of Different Plant Extracts, Plant-Derived Compounds and Synthetic Derivatives of Natural Compounds on Pathogenic Microorganisms, 2nd Volume)
►▼
Show Figures

Figure 1
Open AccessArticle
Lippia graveolens Essential Oil to Enhance the Effect of Imipenem against Axenic and Co-Cultures of Pseudomonas aeruginosa and Acinetobacter baumannii
by
Jorge O. Fimbres-García, Marcela Flores-Sauceda, Elsa Daniela Othón-Díaz, Alfonso García-Galaz, Melvin R. Tapia-Rodriguez, Brenda A. Silva-Espinoza, Andres Alvarez-Armenta and J. Fernando Ayala-Zavala
Antibiotics 2024, 13(5), 444; https://doi.org/10.3390/antibiotics13050444 - 14 May 2024
Abstract
This research focuses on assessing the synergistic effects of Mexican oregano (Lippia graveolens) essential oil or carvacrol when combined with the antibiotic imipenem, aiming to reduce the pathogenic viability and virulence of Acinetobacter baumannii and Pseudomonas aeruginosa. The study highlighted the
[...] Read more.
This research focuses on assessing the synergistic effects of Mexican oregano (Lippia graveolens) essential oil or carvacrol when combined with the antibiotic imipenem, aiming to reduce the pathogenic viability and virulence of Acinetobacter baumannii and Pseudomonas aeruginosa. The study highlighted the synergistic effect of combining L. graveolens essential oil or carvacrol with imipenem, significantly reducing the required doses for inhibiting bacterial growth. The combination treatments drastically lowered the necessary imipenem doses, highlighting a potent enhancement in efficacy against A. baumannii and P. aeruginosa. For example, the minimum inhibitory concentrations (MIC) for the essential oil/imipenem combinations were notably low, at 0.03/0.000023 mg/mL for A. baumannii and 0.0073/0.000023 mg/mL for P. aeruginosa. Similarly, the combinations significantly inhibited biofilm formation at lower concentrations than when the components were used individually, demonstrating the strategic advantage of this approach in combating antibiotic resistance. For OXA-51, imipenem showed a relatively stable interaction during 30 ns of dynamic simulation of their interaction, indicating changes (<2 nm) in ligand positioning during this period. Carvacrol exhibited similar fluctuations to imipenem, suggesting its potential inhibition efficacy, while thymol showed significant variability, particularly at >10 ns, suggesting potential instability. With IMP-1, imipenem also displayed very stable interactions during 38 ns and demonstrated notable movement and positioning changes within the active site, indicating a more dynamic interaction. In contrast, carvacrol and thymol maintained their position within the active site only ~20 and ~15 ns, respectively. These results highlight the effectiveness of combining L. graveolens essential oil and carvacrol with imipenem in tackling the difficult-to-treat pathogens A. baumannii and P. aeruginosa.
Full article
(This article belongs to the Special Issue Essential Oil of the Plants: Chemical Composition, Antimicrobial Activity, and Biological Applications)
►▼
Show Figures

Figure 1
Open AccessArticle
Prevalence and Antimicrobial Resistance Diversity of Salmonella Isolates in Jiaxing City, China
by
Ping Li, Li Zhan, Henghui Wang, Yong Yan, Miaomiao Jia, Lei Gao, Yangming Sun, Guoying Zhu and Zhongwen Chen
Antibiotics 2024, 13(5), 443; https://doi.org/10.3390/antibiotics13050443 - 14 May 2024
Abstract
►▼
Show Figures
Nontyphoidal Salmonella (NTS) is a cause of foodborne diarrheal diseases worldwide. Important emerging NTS serotypes that have spread as multidrug-resistant high-risk clones include S. Typhimurium monophasic variant and S. Kentucky. In this study, we isolated Salmonella in 5019 stool samples collected from patients
[...] Read more.
Nontyphoidal Salmonella (NTS) is a cause of foodborne diarrheal diseases worldwide. Important emerging NTS serotypes that have spread as multidrug-resistant high-risk clones include S. Typhimurium monophasic variant and S. Kentucky. In this study, we isolated Salmonella in 5019 stool samples collected from patients with clinical diarrhea and 484 food samples. Antibiotic susceptibility testing and whole-genome sequencing were performed on positive strains. The detection rates of Salmonella among patients with diarrhea and food samples were 4.0% (200/5019) and 3.1% (15/484), respectively. These 215 Salmonella isolates comprised five main serotypes, namely S. Typhimurium monophasic variant, S. Typhimurium, S. London, S. Enteritidis, and S. Rissen, and were mainly resistant to ampicillin, tetracycline, chloramphenicol, and trimethoprim/sulfamethoxazole. The MDR rates of five major serotypes were 77.4%, 56.0%, 66.7%, 53.3%, and 80.0%, respectively. The most commonly acquired extended-spectrum β-lactamase-encoding genes were blaTEM−1B, blaOXA-10, and blaCTX-M-65. The S. Typhimurium monophasic variant strains from Jiaxing City belonged to a unique clone with broad antibiotic resistance. S. Kentucky isolates showed the highest drug resistance, and all were MDR strains. The discovery of high antibiotic resistance rates in this common foodborne pathogen is a growing concern; therefore, ongoing surveillance is crucial to effectively monitor this pathogen.
Full article

Figure 1
Open AccessSystematic Review
Systematic Review and Meta-Analysis Provide no Guidance on Management of Asymptomatic Bacteriuria within the First Year after Kidney Transplantation
by
José Medina-Polo, Eva Falkensammer, Béla Köves, Jennifer Kranz, Zafer Tandogdu, Ana María Tapia, Tommaso Cai, Florian M. E. Wagenlehner, Laila Schneidewind and Truls Erik Bjerklund Johansen
Antibiotics 2024, 13(5), 442; https://doi.org/10.3390/antibiotics13050442 - 14 May 2024
Abstract
(1) Background: Urinary tract infections (UTIs) are among the most frequent complications in kidney transplant (KT) recipients. Asymptomatic bacteriuria (ASB) may be a risk factor for UTIs and graft rejection. We aimed to evaluate available evidence regarding the benefit of screening and treatment
[...] Read more.
(1) Background: Urinary tract infections (UTIs) are among the most frequent complications in kidney transplant (KT) recipients. Asymptomatic bacteriuria (ASB) may be a risk factor for UTIs and graft rejection. We aimed to evaluate available evidence regarding the benefit of screening and treatment of ASB within the first year after KT. (2) Evidence acquisition: A systematic literature search was conducted in MEDLINE, the Cochrane Library CENTRAL and Embase. Inclusion criteria were manuscripts in English addressing the management of ASB after KT. The PICO questions concerned Patients (adults receiving a KT), Intervention (screening, diagnosis and treatment of ASB), Control (screening and no antibiotic treatment) and Outcome (UTIs, sepsis, kidney failure and death). (3) Evidence synthesis: The systematic review identified 151 studies, and 16 full-text articles were evaluated. Seven were excluded because they did not evaluate the effect of treatment of ASB. There was no evidence for a higher incidence of lower UTIs, acute pyelonephritis, graft loss, or mortality in patients not treated with antibiotics for ASB. Analysis of comparative non-randomized and observational studies did not provide supplementary evidence to guide clinical recommendations. We believe this lack of evidence is due to confounding risk factors that are not being considered in the stratification of study patients.
Full article
(This article belongs to the Special Issue Antimicrobial Prescribing and Antimicrobial Use in Healthcare Settings)
►▼
Show Figures

Figure 1
Open AccessArticle
Antimicrobial Properties of Newly Developed Silver-Enriched Red Onion–Polymer Composites
by
Judita Puišo, Jonas Žvirgždas, Algimantas Paškevičius, Shirin Arslonova and Diana Adlienė
Antibiotics 2024, 13(5), 441; https://doi.org/10.3390/antibiotics13050441 - 14 May 2024
Abstract
Simple low-cost, nontoxic, environmentally friendly plant-extract-based polymer films play an important role in their application in medicine, the food industry, and agriculture. The addition of silver nanoparticles to the composition of these films enhances their antimicrobial capabilities and makes them suitable for the
[...] Read more.
Simple low-cost, nontoxic, environmentally friendly plant-extract-based polymer films play an important role in their application in medicine, the food industry, and agriculture. The addition of silver nanoparticles to the composition of these films enhances their antimicrobial capabilities and makes them suitable for the treatment and prevention of infections. In this study, polymer-based gels and films (AgRonPVA) containing silver nanoparticles (AgNPs) were produced at room temperature from fresh red onion peel extract (“Ron”), silver nitrate, and polyvinyl alcohol (PVA). Silver nanoparticles were synthesized directly in a polymer matrix, which was irradiated by UV light. The presence of nanoparticles was approved by analyzing characteristic local surface plasmon resonance peaks occurring in UV-Vis absorbance spectra of irradiated experimental samples. The proof of evidence was supported by the results of XRD and EDX measurements. The diffusion-based method was applied to investigate the antimicrobial activity of several types of microbes located in the environment of the produced samples. Bacteria Staphylococcus aureus ATCC 29213, Acinetobacter baumannii ATCC BAA 747, and Pseudomonas aeruginosa ATCC 15442; yeasts Candida parapsilosis CBS 8836 and Candida albicans ATCC 90028; and microscopic fungi assays Aspergillus flavus BTL G-33 and Aspergillus fumigatus BTL G-38 were used in this investigation. The greatest effect was observed on Staphylococcus aureus, Acinetobacter baumannii, and Pseudomonas aeruginosa bacteria, defining these films as potential candidates for antimicrobial applications. The antimicrobial features of the films were less effective against fungi and the weakest against yeasts.
Full article
(This article belongs to the Special Issue Silver and Gold Compounds as Antibiotics)
►▼
Show Figures

Figure 1
Open AccessSystematic Review
One- vs. Two-Stage Revision for Periprosthetic Shoulder Infections: A Systematic Review and Meta-Analysis
by
Mohamad Bdeir, Aimée Lerchl, Svetlana Hetjens, Andreas Schilder, Sascha Gravius, Tobias Baumgärtner and Ali Darwich
Antibiotics 2024, 13(5), 440; https://doi.org/10.3390/antibiotics13050440 - 14 May 2024
Abstract
Periprosthetic shoulder infection (PSI) remains a challenging complication after shoulder arthroplasty. Therapeutic options include one- or two-stage revision, irrigation and debridement, and resection arthroplasty. With our systematic review and meta-analysis, we aimed to compare one- and two-stage revisions for periprosthetic shoulder joint infections
[...] Read more.
Periprosthetic shoulder infection (PSI) remains a challenging complication after shoulder arthroplasty. Therapeutic options include one- or two-stage revision, irrigation and debridement, and resection arthroplasty. With our systematic review and meta-analysis, we aimed to compare one- and two-stage revisions for periprosthetic shoulder joint infections and determine the most appropriate therapeutic procedure. We performed an extensive literature search in PubMed, Ovid Medline, Cochrane Library, Web of Science, and CINAHL and filtered out all relevant studies. The meta-analysis was performed using the random-effects model, heterogeneity was analyzed using I2, and publication bias was assessed using the Egger’s test. A total of 8 studies with one-stage revisions, 36 studies with two-stage revisions, and 12 studies with both one-stage and two-stage revisions were included. According to the random-effects model, the reinfection rate for the entirety of the studies was 12.3% (95% Cl: 9.6–15.3), with a low-to-moderate heterogeneity of I2 = 47.72%. The reinfection rate of the one-stage revisions was 10.9%, which was significantly lower than the reinfection rate of the two-stage revisions, which was 12.93% (p = 0.0062). The one-stage revision rate was significantly lower with 1.16 vs. 2.25 revisions in the two-stage revision group (p < 0.0001). The postoperative functional outcome in one-stage-revised patients was comparable but not statistically significant (p = 0.1523). In one- and two-stage revisions, most infections were caused by Cutibacterium acnes. In summary, our systematic review and meta-analysis show the superiority of single-stage revision regarding reinfection and revision rates in periprosthetic shoulder joint infection.
Full article
(This article belongs to the Special Issue Antibiotics in Orthopedic Infections, 2nd Volume)
►▼
Show Figures

Figure 1
Open AccessReview
AMPs as Host-Directed Immunomodulatory Agents against Skin Infections Caused by Opportunistic Bacterial Pathogens
by
Subhasree Saha, Devashish Barik and Debabrata Biswas
Antibiotics 2024, 13(5), 439; https://doi.org/10.3390/antibiotics13050439 - 13 May 2024
Abstract
Skin is the primary and largest protective organ of the human body. It produces a number of highly evolved arsenal of factors to counter the continuous assault of foreign materials and pathogens from the environment. One such potent factor is the repertoire of
[...] Read more.
Skin is the primary and largest protective organ of the human body. It produces a number of highly evolved arsenal of factors to counter the continuous assault of foreign materials and pathogens from the environment. One such potent factor is the repertoire of Antimicrobial Peptides (AMPs) that not only directly destroys invading pathogens, but also optimally modulate the immune functions of the body to counter the establishment and spread of infections. The canonical direct antimicrobial functions of these AMPs have been in focus for a long time to design principles for enhanced therapeutics, especially against the multi-drug resistant pathogens. However, in recent times the immunomodulatory functions performed by these peptides at sub-microbicidal concentrations have been a point of major focus in the field of host-directed therapeutics. Such strategies have the added benefit of not having the pathogens develop resistance against the immunomodulatory pathways, since the pathogens exploit these signaling pathways to obtain and survive within the host. Thus, this review summarizes the potent immunomodulatory effect of these AMPs on, specifically, the different host immune cells with the view of providing a platform of information that might help in designing studies to exploit and formulate effective host-directed adjunct therapeutic strategies that would synergies with drug regimens to counter the current diversity of drug-resistant skin opportunistic pathogens.
Full article
(This article belongs to the Special Issue Antimicrobial Peptides: A New Hope in the War against Multi-Drug Resistance)
►▼
Show Figures

Figure 1
Open AccessEditorial
Antibiotic Use in Communities
by
Timo J. Lajunen
Antibiotics 2024, 13(5), 438; https://doi.org/10.3390/antibiotics13050438 - 13 May 2024
Abstract
Since their discovery and clinical introduction in the 1930s–1940s, penicillin and sulphonamides have had a profound impact on public health [...]
Full article
(This article belongs to the Special Issue Feature Papers in Antibiotic Use in the Communities)
Open AccessArticle
A Response Surface Methodological Approach for Large-Scale Production of Antibacterials from Lactiplantibacillus plantarum with Potential Utility against Foodborne and Orthopedic Infections
by
Paulpandian Prema, Daoud Ali, Van-Huy Nguyen, Bhathini Vaikuntavasan Pradeep, Veeramani Veeramanikandan, Maria Daglia, Carla Renata Arciola and Paulraj Balaji
Antibiotics 2024, 13(5), 437; https://doi.org/10.3390/antibiotics13050437 - 13 May 2024
Abstract
A variety of bacteria, including beneficial probiotic lactobacilli, produce antibacterials to kill competing bacteria. Lactobacilli secrete antimicrobial peptides (AMPs) called bacteriocins and organic acids. In the food industry, bacteriocins, but even whole cell-free supernatants, are becoming more and more important as bio-preservatives, while,
[...] Read more.
A variety of bacteria, including beneficial probiotic lactobacilli, produce antibacterials to kill competing bacteria. Lactobacilli secrete antimicrobial peptides (AMPs) called bacteriocins and organic acids. In the food industry, bacteriocins, but even whole cell-free supernatants, are becoming more and more important as bio-preservatives, while, in orthopedics, bacteriocins are introducing new perspectives in biomaterials technologies for anti-infective surfaces. Studies are focusing on Lactiplantibacillus plantarum (previously known as Lactobacillus plantarum). L. plantarum exhibits great phenotypic versatility, which enhances the chances for its industrial exploitation. Importantly, more than other lactobacilli, it relies on AMPs for its antibacterial activity. In this study, Response Surface Methodology (RSM) through a Box–Behnken experimental design was used to estimate the optimal conditions for the production of antibacterials by L. plantarum. A temperature of 35 °C, pH 6.5, and an incubation time of 48 h provided the highest concentration of antibacterials. The initial pH was the main factor influencing the production of antibacterials, at 95% confidence level. Thanks to RSM, the titer of antibacterials increased more than 10-fold, this result being markedly higher than those obtained in the very few studies that have so far used similar statistical methodologies. The Box–Behnken design turned out to be a valid model to satisfactorily plan a large-scale production of antibacterials from L. plantarum.
Full article
(This article belongs to the Special Issue Development and Biomedical Application of Antibacterial Coatings)
►▼
Show Figures

Figure 1
Open AccessReview
A Comparison of Currently Available and Investigational Fecal Microbiota Transplant Products for Recurrent Clostridioides difficile Infection
by
Yifan Wang, Aaron Hunt, Larry Danziger and Emily N. Drwiega
Antibiotics 2024, 13(5), 436; https://doi.org/10.3390/antibiotics13050436 - 12 May 2024
Abstract
Clostridioides difficile infection (CDI) is an intestinal infection that causes morbidity and mortality and places significant burden and cost on the healthcare system, especially in recurrent cases. Antibiotic overuse is well recognized as the leading cause of CDI in high-risk patients, and studies
[...] Read more.
Clostridioides difficile infection (CDI) is an intestinal infection that causes morbidity and mortality and places significant burden and cost on the healthcare system, especially in recurrent cases. Antibiotic overuse is well recognized as the leading cause of CDI in high-risk patients, and studies have demonstrated that even short-term antibiotic exposure can cause a large and persistent disturbance to human colonic microbiota. The recovery and sustainability of the gut microbiome after dysbiosis have been associated with fewer CDI recurrences. Fecal microbiota transplantation (FMT) refers to the procedure in which human donor stool is processed and transplanted to a patient with CDI. It has been historically used in patients with pseudomembranous colitis even before the discovery of Clostridioides difficile. More recent research supports the use of FMT as part of the standard therapy of recurrent CDI. This article will be an in-depth review of five microbiome therapeutic products that are either under investigation or currently commercially available: Rebyota (fecal microbiota, live-jslm, formerly RBX2660), Vowst (fecal microbiota spores, live-brpk, formerly SER109), VE303, CP101, and RBX7455. Included in this review is a comparison of the products’ composition and dosage forms, available safety and efficacy data, and investigational status.
Full article
(This article belongs to the Special Issue The Control of Gut Microbiota: Antibiotics Alternatives and Fecal Microbiota Transplantation)
Open AccessArticle
Carbapenem-Resistant NDM and OXA-48-like Producing K. pneumoniae: From Menacing Superbug to a Mundane Bacteria; A Retrospective Study in a Romanian Tertiary Hospital
by
Dragos Stefan Lazar, Maria Nica, Amalia Dascalu, Corina Oprisan, Oana Albu, Daniel Romeo Codreanu, Alma Gabriela Kosa, Corneliu Petru Popescu and Simin Aysel Florescu
Antibiotics 2024, 13(5), 435; https://doi.org/10.3390/antibiotics13050435 - 12 May 2024
Abstract
Background: Carbapenem-resistant Klebsiella pneumoniae (Cr-Kpn) is becoming a growing public health problem through the failure of adequate treatment. This study’s objectives are to describe the sources of Cr-Kpn in our hospital over 22 months, associating factors with the outcome of Cr-Kpn-positive patients, especially
[...] Read more.
Background: Carbapenem-resistant Klebsiella pneumoniae (Cr-Kpn) is becoming a growing public health problem through the failure of adequate treatment. This study’s objectives are to describe the sources of Cr-Kpn in our hospital over 22 months, associating factors with the outcome of Cr-Kpn-positive patients, especially those with NDM+OXA-48-like (New Delhi Metallo-β-Lactamase and oxacillinase-48), and the effectiveness of the treatments used. Methods: A retrospective observational cohort study including all hospitalized patients with Cr-Kpn isolates. We reported data as percentages and identified independent predictors for mortality over hospital time through multivariate analysis. Results: The main type of carbapenemases identified were NDM+OXA-48-like (49.4%). The statistical analysis identified that diabetes and co-infections with the Gram-negative, non-urinary sites of infection were factors of unfavorable evolution. The Cox regression model identified factors associated with a poor outcome: ICU admission (HR of 2.38), previous medical wards transition (HR of 4.69), and carbapenemase type NDM (HR of 5.98). We did not find the superiority of an antibiotic regimen, especially in the case of NDM+OXA-48-like. Conclusions: The increase in the incidence of Cr-Kpn infections, especially with NDM+OXA-48-like pathogens, requires a paradigm shift in both the treatment of infected patients and the control of the spread of these pathogens, which calls for a change in public health policy regarding the use of antibiotics and the pursuit of a One Health approach.
Full article
(This article belongs to the Special Issue United in the Prevention of Bacterial Resistance during the Post-pandemic Era)
►▼
Show Figures

Figure 1
Open AccessArticle
Inhibition of Candida albicans Biofilm Formation and Attenuation of Its Virulence by Liriope muscari
by
Jeonghoon Lee, Hyunchan Song and Kiyoung Kim
Antibiotics 2024, 13(5), 434; https://doi.org/10.3390/antibiotics13050434 - 12 May 2024
Abstract
(1) Background: Although Candida albicans accounts for the majority of fungal infections, therapeutic options are limited and require alternative antifungal agents with new targets; (2) Methods: A biofilm formation assay with RPMI1640 medium was performed with Liriope muscari extract. A combination antifungal assay,
[...] Read more.
(1) Background: Although Candida albicans accounts for the majority of fungal infections, therapeutic options are limited and require alternative antifungal agents with new targets; (2) Methods: A biofilm formation assay with RPMI1640 medium was performed with Liriope muscari extract. A combination antifungal assay, dimorphic transition assay, and adhesion assay were performed under the biofilm formation condition to determine the anti-biofilm formation effect. qRT-PCR analysis was accomplished to confirm changes in gene expression; (3) Results: L. muscari extract significantly reduces biofilm formation by 51.65% at 1.56 μg/mL use and therefore increases susceptibility to miconazole. L. muscari extract also inhibited the dimorphic transition of Candida; nearly 50% of the transition was inhibited when 1.56 μg/mL of the extract was treated. The extract of L. muscari inhibited the expression of genes related to hyphal development and extracellular matrix of 34.4% and 36.0%, respectively, as well as genes within the Ras1-cAMP-PKA, Cph2-Tec1, and MAP kinase signaling pathways of 25.58%, 7.1% and 15.8%, respectively, at 1.56 μg/mL of L. muscari extract treatment; (4) Conclusions: L. muscari extract significantly reduced Candida biofilm formation, which lead to induced antifungal susceptibility to miconazole. It suggests that L. muscari extract is a promising anti-biofilm candidate of Candida albicans since the biofilm formation of Candida albicans is an excellent target for candidiasis regulation.
Full article
(This article belongs to the Special Issue Antibiofilm Activity against Multidrug-Resistant Pathogens)
►▼
Show Figures

Figure 1
Open AccessArticle
Macrolide Resistance in the Aerococcus urinae Complex: Implications for Integrative and Conjugative Elements
by
Jyoti Lamichhane, Brian I. Choi, Natalie Stegman, Melline Fontes Noronha and Alan J. Wolfe
Antibiotics 2024, 13(5), 433; https://doi.org/10.3390/antibiotics13050433 - 10 May 2024
Abstract
The recognition of the Aerococcus urinae complex (AUC) as an emerging uropathogen has led to growing concerns due to a limited understanding of its disease spectrum and antibiotic resistance profiles. Here, we investigated the prevalence of macrolide resistance within urinary AUC isolates, shedding
[...] Read more.
The recognition of the Aerococcus urinae complex (AUC) as an emerging uropathogen has led to growing concerns due to a limited understanding of its disease spectrum and antibiotic resistance profiles. Here, we investigated the prevalence of macrolide resistance within urinary AUC isolates, shedding light on potential genetic mechanisms. Phenotypic testing revealed a high rate of macrolide resistance: 45%, among a total of 189 urinary AUC isolates. Genomic analysis identified integrative and conjugative elements (ICEs) as carriers of the macrolide resistance gene ermA, suggesting horizontal gene transfer as a mechanism of resistance. Furthermore, comparison with publicly available genomes of related pathogens revealed high ICE sequence homogeneity, highlighting the potential for cross-species dissemination of resistance determinants. Understanding mechanisms of resistance is crucial for developing effective surveillance strategies and improving antibiotic use. Furthermore, the findings underscore the importance of considering the broader ecological context of resistance dissemination, emphasizing the need for community-level surveillance to combat the spread of antibiotic resistance within the urinary microbiome.
Full article
(This article belongs to the Special Issue Uropathogens—Antibiotic Resistance and Alternative Therapies, 2nd Edition)
►▼
Show Figures
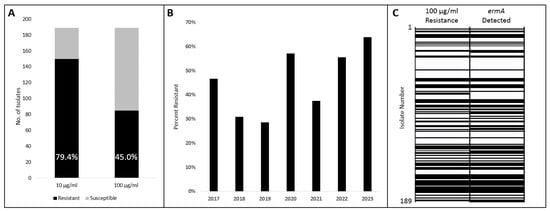
Figure 1

Journal Menu
► ▼ Journal Menu-
- Antibiotics Home
- Aims & Scope
- Editorial Board
- Reviewer Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Sections & Collections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Conferences
- Editorial Office
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Antibiotics, Antioxidants, JoF, Microbiology Research, Microorganisms
Redox in Microorganisms, 2nd Edition
Topic Editors: Michal Letek, Volker BehrendsDeadline: 31 July 2024
Topic in
Antibiotics, JPM, Pharmaceuticals, Pharmaceutics
Pharmacokinetic and Pharmacodynamic Modelling in Drug Discovery and Development
Topic Editors: Inaki F. Troconiz, Victor Mangas Sanjuán, Maria Garcia-Cremades MiraDeadline: 31 August 2024
Topic in
Molecules, Pharmaceutics, Antibiotics, Microorganisms, Biomolecules, Marine Drugs, Polymers, IJMS
Antimicrobial Agents and Nanomaterials
Topic Editors: Sandra Pinto, Vasco D. B. BonifácioDeadline: 30 September 2024
Topic in
Antibiotics, Biomedicines, JCM, Pharmaceuticals, Pharmaceutics
Challenges and Future Prospects of Antibacterial Therapy
Topic Editors: Kwang-sun Kim, Zehra EdisDeadline: 31 October 2024

Conferences
Special Issues
Special Issue in
Antibiotics
Antibacterial Treatment in Periodontal and Endodontic Therapy, 2nd Volume
Guest Editors: Andreas Braun, Felix KrauseDeadline: 15 May 2024
Special Issue in
Antibiotics
The Application of Antibiotic Therapy in Oral Surgery and Dental Implant Procedures
Guest Editors: Eugenio Velasco-Ortega, Angel-Orion Salgado-Peralvo, Juan Francisco Peña-CardellesDeadline: 31 May 2024
Special Issue in
Antibiotics
Challenges for Therapeutic Drug Monitoring of Antimicrobials
Guest Editors: Giuseppe Pipitone, Giuseppe Nunnari, Fabrizio TagliettiDeadline: 15 June 2024
Special Issue in
Antibiotics
Antimicrobial Drug Discovery: New Theories and New Therapies
Guest Editor: Ki-Young KimDeadline: 30 June 2024
Topical Collections
Topical Collection in
Antibiotics
Antimicrobial Resistance and Anti-Biofilms
Collection Editors: Ding-Qiang Chen, Yulong Tan, Ren-You Gan, Guanggang Qu, Zhenbo Xu, Junyan Liu









